MRI findings in Marion's disease: the bulb and the doughnut signs
(Download pdf)
Ernesto Lima Araujo Melo, Ligia Persici Rodrigues, Ricardo Reges Maia de Oliveira
Centro Avançado de Diagnóstico por Imagem (Boghos Dom Luis), (ELAM), Instituto Dr. José Frota (LPR) and Faculdade de Medicina Christus & Faculdade de Medicina da Universidade Federal do Ceará (RRMO), Fortaleza, CE, Brazil
Radiology Page
Vol. 38 (6): 855-856, November - December, 2012
A 77-year-old female presented to our facility with a five-year history of progressive urinary bladder retention and voiding difficulties. She underwent a pelvic magnetic resonance imaging (MRI) examination as a part of her lower urinary tract symptoms evaluation, and for treatment planning.
MRI with a torso phased-array superficial coil was performed in a 1.5T magnetic field equipment. We obtained multiplanar T1- and T2-weighted pre-contrast sequences, with and without fat suppression techniques, axial diffusion weighted images, axial apparent diffusion coefficient (ADC) map, and multiplanar T1-weighted fat suppressed images after the administration of intravenous gadolinium.
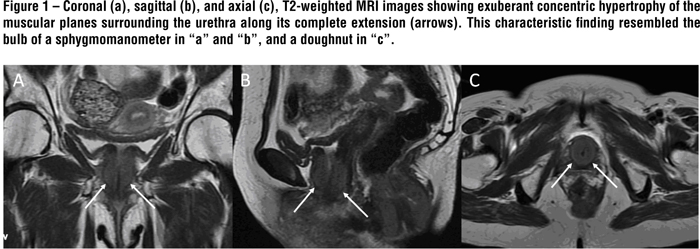
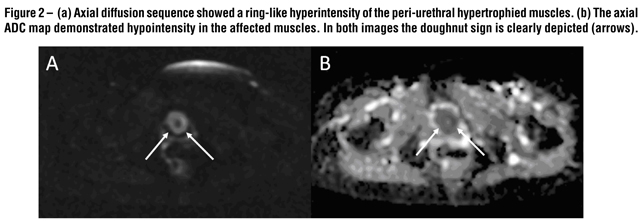
MRI revealed an exuberant concentric hypertrophy of the entire urethra. This characteristic imaging finding resembled a bulb of a sphygmomanometer on the sagittal and coronal planes, and a doughnut on the axial ones (Figure-1). The affected musculature was isointense on T1- and slightly hyperintense on T2-weighted images compared with unaffected muscles. The diffusion sequence showed restriction to free water molecules movements, making the hypertrophied muscles hyperintense on this sequence and hypointense on the ADC map (Figure-2). Additionally this patient also exhibited a marked concentric hypertrophy of the internal anal sphincter muscle, probably related to the same bladder neck neuropathological mechanism. This latter finding was previously misdiagnosed in another facility as a rectal tumor. After the intravenous contrast administration, there was slight enhancement of the hypertrophied muscle. The combination of the MRI findings together with the patient´s symptoms and urodynamic testing was consistent with the diagnosis of primary bladder neck obstruction (PBNO) due to severe muscular hypertrophy.
Discussion
PBNO was first described in men by Marion1, a condition wherein the bladder neck fails to open adequately during voiding, resulting in increased striated sphincter activity or obstruction of urinary flow in the absence of another anatomic obstruction, such as that caused by benign prostatic enlargement in men or genitourinary prolapse in women.2,3
Men typically present with symptoms for years before a correct diagnosis of PBNO is made. PBNO can present with a variety of symptoms including voiding or obstructive symptoms (decreased force of stream, hesitancy, intermittent stream, incomplete emptying), storage or irritative symptoms (frequency, urgency, urge incontinence, nocturia), or a combination of both. Occasionally, the initial presentation may be urinary retentions.3 Presenting symptoms appear to be similar in men and women, with a combination of voiding and storage symptoms being common.4 Currently PBNO is diagnosed primarily by videourodynamics and cystourethroscopy, but the increasing use of MRI can introduce new imaging findings.5
List of Abbreviations
- ADC: axial apparent diffusion coefficient
- MRI: magnetic resonance imaging
- PBNO: primary bladder neck obstruction
References
- Marion G. Surgery of the neck of the bladder. Br J Urol. 1933; 5:351-357.
- Nitti VW. Primary bladder neck obstruction in men and women. Rev Urol. 2005; 7(suppl 8): S12-S17.
- Huckabay C, Nitti VW. Diagnosis and treatment of primary bladder neck obstruction in men. Curr Urol Rep. 2005; 6(4):271-275.
- Dewan PA, Rajimwale A, Gent RJ, Lequesne GW. Marion´s disease presenting as prenatal hydronephrosis. Pediatr Surg Int. 1994; 9:290-292.
- N Tasali, Cubuk R, Sinanoglu O, Sahin K, Saydam B. MRI in stress urinary incontinence: endovaginal MRI with an intracavitary coil and dynamic pelvic MRI. Urol J. 2012; 9(1):397-404.
________________________
Correspondence address:
Dr. Ernesto Lima Araujo Melo
Av. Dom Luis, 1233 / 1809
Fortaleza, CE, 60160-230, Brazil
Telephone: + 55 85 9906-7760
E-mail: contato@ernestomelo.med.br