PENILE
FRACTURE - EXPERIENCE IN 56 CASES
(
Download pdf )
LEANDRO KOIFMAN, ANDRÉ G. CAVALCANTI, CARLOS HENRIQUE MANES, DAIBES R. FILHO, LUCIANO A. FAVORITO
Division of Urology, Souza Aguiar Municipal Hospital, Rio de Janeiro, RJ, Brazil
ABSTRACT
Objective:
The aim of this work is to report the diagnostic and therapeutic options
for 55 patients with clinical diagnosis of penile fracture.
Material and Methods: The patients were
retrospectively assessed between 1982 and 2002. The primary diagnostic
evaluation method for 55 patients (56 fractures) was clinical history
and physical exam. Ten (17.8%) cases required complementary exams. Ultrasound
(US) was performed in 2 cases, and magnetic resonance imaging (MRI) in
1 case. Retrograde urethrocystogram was performed in suspicious urethral
injury, which happened for 7 patients.
Results: Of 56 assessed cases, 49 (89.5%)
were submitted to surgical exploration, and only 7 were conservatively
conducted. Surgical treatment was performed in 48 patients (49 fractures),
in these cases, 47 (95.9%) presented tunica albuginea disruption and solely
2 (4.1%) evidenced lesion of dorsal vein. Ultrasonography confirmed disruption
of tunica albuginea in 1 (50%) case, and in the other it was not possible
to determinate the origin of the lesion, and the patient was submitted
to surgical exploration, which confirmed the condition. MRI was used only
in 1 case, confirming the lesion. Among 7 patients submitted to conservative
management, until now, 3 (42.8%) required surgical intervention to correct
penile chordee.
Conclusions: Penile fracture is an entity
of eminently clinical diagnosis, which management should be surgical and
immediate, avoiding thus complications related to erectile dysfunction.
When suspecting an associated urethral injury, Urethrocystogram is recommended.
In cases where there is diagnostic uncertainty, ultrasound and/or MRI
may be used to reveal the condition.
Key words:
penis; urethra; fractures; therapeutics; surgery
Int Braz J Urol. 2003; 29: 35-9
INTRODUCTION
Penile
fracture is one of the less frequent urological traumas. There are 183
reports about this subject published, with 1,331 cases described from
1935 to 2001 (1). It is defined as a rupture of the corpus cavernosum
due to a blunt trauma in an erect penis. Lesions on a flaccid penis or
lesions in the suspensor ligament of the penis are not included in this
definition (2).
Vaginal intercourse is the most common cause
of penile fractures (1,3-5), masturbation is also reported as a cause
of penile fracture (6). In lower incidence, the lesion could occur during
a nocturnal erection due to the patient rolling over his own body.
Penile fracture has a quite typical clinical
presentation. Patients report hearing a snap sound followed by pain, penile
detumescence, and late appearing swelling, hematoma and penile deformity
(7-9). In the presence of associated urethral injury, happening in 10%
to 20% of the cases, findings as urethral bleeding, hematuria and difficulty
voiding may be observed (8,10).
There are several reports about management
and complications in patients with penile fracture; yet, studies with
longer follow-up, and reports about ultrasound and MRI use as diagnostic
tools are uncommon.
The aim of this paper is to report the experience
of 56 cases assessed in 55 patients, admitted to our facility with a clinical
diagnosis of penile fracture in the last 20 years, and discuss the therapeutic
and diagnostic options to this type of lesion.
MATERIALS AND METHODS
In
the period between January 1982 and May 2002, 55 patients (56 fractures—the
same patient having had 2 fractures in a 90 days interval) with clinical
diagnosis of penile fracture were admitted in our facility and retrospectively
assessed. Patients’ age ranged from 18 and 63 years (mean 33 years).
Sexual trauma was the most common cause corresponding to 53 (94.7%) cases,
followed by lesion due to penis manipulation in 3 (5.3%) cases. Time elapsed
form the trauma to the arrival at the hospital ranged from 2 hours to
3 weeks (mean 14 hours).
Primary diagnostic assessment was clinical
history and physical exam (Figure-1). In 10 (17.8%) cases, complementary
exams were required. Ultrasound scan was used in 2 cases and MRI in 1
case. Retrograde urethrocystogram was performed solely when urethral injury
was suspected, what happened to 7 patients.

SURGICAL TECHNIQUE
The
surgical technique used consisted of a subcoronal incision, with penile
degloving and exposure of the corpora cavernosum and urethra. Bladder
catheterization was routinely performed, except for the cases where a
urethral injury was suspected. All corpora cavernosa lesions identified
during surgical exploration were treated by interrupted polyglactine 3-0
sutures. Urethral lesions were primarily corrected with interrupted absorbable
polyglactine 5-0 sutures. Bladder catheter was maintained during 12 hours
after the surgical procedure conclusion for patients without urethral
lesions; 7-10 days in patients with partial urethral injury; and 14-21
days in patients with total urethral section.
Only 1 patient required Penrose #1 drain
owing to the severity of the lesion (bilateral albuginea disruption and
total urethral section), and the presence of a large hematoma. The drain
was withdrawn at hospital discharge.
RESULTS
From
56 cases assessed, 49 (87.5%) were submitted to surgical exploration,
and only 7 (12.5%) were conservatively managed. Table-1 shows lesions
observed during surgical exploration.
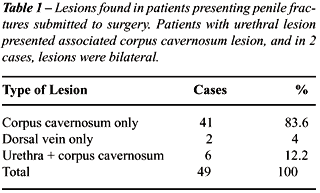
From 48 patients (49 fractures) submitted
to surgical procedure, 47 (95.9%) presented disruption of tunica albuginea
and only 2 (4.1%) showed lesion of the dorsal vein (Figure-2). In 6 (12.2%)
patients urethral injury occurred, and in all these we found associated
corpus cavernosum lesions.

From 47 penile fracture cases, with albuginea
disruption, 45 (95.7%) presented unilateral lesion, and 2 (4.3%) bilateral
lesion. Both cases of bilateral corpora cavernosa lesion were associated
to urethral injury. Lesion size ranged from 0.3 cm to 4.0 cm (mean 1.5
cm).
In the group of patients submitted to surgical
exploration, 32 had follow-up longer than 1 year. In this group, there
was no complaint about erectile dysfunction after the trauma, and only
2 (6.2%) patients developed slight penile curvature, without sexual function
impairment.
We have observed urethral bleeding and difficulty
voiding in 7 (12.5%) cases, for which Urethrocystogram was performed,
evidencing contrast medium leakage in 6 cases. After their surgical exploration,
the urethral injury was confirmed in all 6 cases, demonstrating the exam
accuracy. Of 6 patients with confirmed diagnosis of urethral injury, only
1 had total lesion. Among these patients, 4 presented unilateral corpus
cavernosum lesion, and 2 presented bilateral lesion.
Ultrasound study confirmed an albuginea
disruption in 1 (50%) case, in the other, it was not possible to determine
the lesion, and the patient was submitted to surgical exploration that
confirmed the condition. MRI was used in only 1 case, confirming the lesion
(Figure-3).

Among 7 patients conservatively managed
(treatment decided by the urologist during the admission), until nowadays
3 (42.8%) needed surgical procedures to correct the penile chordee.
DISCUSSION
There
are few reports with a significant series about penile fracture in the
literature (11). Penile fracture is an entity that generally has its diagnosis
confirmed by its clinical presentation. The typical history, associated
with physical exam findings, exempts performing complementary exams. For
the rare exceptions where there is diagnostic uncertainty, some imaging
methods may be used.
Ultrasound has a limited role in the diagnosis
of penile fracture (12-14). As it is an examiner-depending method, for
which interpreting depends on the examiner’s experience, rareness
of these lesions often precludes an accurate diagnosis (12). Small albuginea
disruptions and the presence of clots at the place where fracture site
occurred may easily be unperceived (12-15).
In both cases assessed by ultrasound, albuginea
disruption was observed only in 1 patient. However, as it is a non-invasive
method, with low cost and accessible in the great majority of institutions,
it may help to evaluate uncertain cases.
Magnetic resonance imaging has been also
used for demonstrating corpus cavernosum lesions (11,12,16,17). Its high
accuracy can discriminate the intensity of corpora cavernosa vascular
sinusoids (high intensity) relative to tunica albuginea (low intensity),
allowing for accurate diagnosis (12,16,17). Nevertheless, it is a high-cost
exam, and it is not available at most institutions. In our series, only
1 patient (with diagnostic uncertainty) was submitted to this exam, with
an accurate confirmation of the lesion.
In suspicion of urethral injury, an urethrocystogram
shall be performed. As it is a low-cost exam, easy to perform and highly
accurate, all patients with an urethral injury suspected were submitted
to the exam. Of 7 cases assessed, 6 presented contrast medium leakage.
After surgical exploration, urethral injury was confirmed for all 6 cases.
However, it is worth remembering that, in other published series, Urethrocystogram
did not demonstrate this efficiency, being thus criticized by some authors
(8,18).
Previous studies report 10% to 41% complications
rates from conservative management of penile fracture, and surgical treatment
is, thus, the main option for this type of trauma (4,6,7,11,12,18-20).
We have observed medical complications for 37.5% of conservatively managed
patients, supporting the data presented in previous publications. In our
series, none of surgically treated patients presented penile curvature
during pos-operative period, a relatively infrequent complication that
generally does not affect sexual intercourse (21).
During sexual intercourse the rupture of
dorsal vein of the penis may occur, leading to a clinical presentation
similar to penile fracture (22). Differentiating these 2 types of trauma
sometimes is possible only through surgical exploration, which is the
treatment of choice for both conditions. Among 56 cases in our series,
only 2 presented dorsal vein of penis lesion.
Disagreement about the type of incision
to be used in treating penile fracture remains. Longitudinal incisions
over the area where the fracture is suspected, parapenile incisions exposing
shaft or even inguino-scrotal incisions were proposed (23-25). Penile
deglovement, however, offers a better exposure, in addition to allowing
evaluation of both corpora cavernosa and corpus spongiosum.
CONCLUSIONS
Penile
fracture is an entity which diagnosis is eminently clinical, and its management
should be surgical and immediate, avoiding thus complications related
to erectile dysfunction.
In suspicious of urethral injury, Urethrocystogram
is recommended. In cases where there is diagnostic uncertainty, an ultrasound
and/or magnetic resonance imaging may be use to reveal the condition.
REFERENCES
- Eke N: Fracture o the penis. Br J Surg. 2002; 89:555-65.
- El-Sherif AE, Dauleh M, Allowneh N, Vijayan P: Management of fracture of the penis in Quatar. Br J Urol. 1991; 68:622-5.
- Schonberger B: Verletzungen der mannlichen Genitalorgane. Z Urol Nephrol. 1982; 5:879-83.
- Nicoliasen S, Melamud A, McAninch JW: Rupture of the corpus cavernosum: Surgical management. J Urol. 1983; 130:917-20.
- Klein FA, Smith V, Miller N: Penile fracture: Diagnosis and management. J Trauma 1985; 25:1090-2.
- Taha SA, Sharayah A, Kamal BA, Salem AA, Khwaja S: Fracture of the penis: Surgical manegement. Int Surg. 1988; 73:63-4.
- Meares EM: Traumatic rupture of the corpus cavernosum. J Urol. 1971; 105:407-9.
- Mydlo JH, Hayyeri M, Macchia RJ: Uretrography and cavernosography imaging in a small series of penile fractures: a comparison with surgical findings. Urology 1998; 51:616-9.
- Ruckle CH, Hadley HR, Lui PD: Fracture of the penis: Diagnosis and manegement. Urology 1992; 40:33-5.
- Tsang T, Demby AM: Penile fracture with urethral injury. J Urol. 1992; 147:466-8.
- Zargooshi J: Penile fracture in Kermanshah, Iran: report of 172 cases. J Urol. 2000; 164:364-6.
- Miller S, McAninch JW: Penile Fracture and Soft Tissue Injury. In: Traumatic and Reconstructive Urology. Edited by J.W. McAninch. Philadelphia, W.B. Saunders, 1996; chapt. 59, pp.693–8.
- Dierks PR, Hawkins H: Sonography and penile trauma. J Ultrasound Med. 1983; 2: 417-9.
- Martinez Perez E, Arnaiz Esteban F: Fracture of the penis: two new cases. Review of the literature: usefulness of ecography. Arch Esp Urol. 1997; 50:1099-102.
- Hoekx L: Fracture of the penis: role of ultrassonography in localizing tear. Acta Urol Belg. 1998; 66:23-5.
- Fedel M, Venz S, Andressen R, Sudhoff F, Loening S: The value of magnetic ressonance imaging in the diagnosis of suspected penile fracture with atypical clinical findings. J Urol. 1996; 155:1924-7.
- Susuki K, Shimizu N, Kurokawa K, Susuki T, Yamanaka H: Fracture of the penis: magnetic ressonance imaging of the rupture of the corpus cavernosum. Br J Urol. 1995; 76:803-4.
- Gianini PTR, Piovesan ACP, Mesquita JLB, Romao RLP, Arap S: Long-term outcome of penile fracture treatment. Int Braz J Urol. 2001; 27:46-9.
- Pryor JP, Hill JT, Packham DA, Yates-Bell AJ: Penile injuries with particular reference to injury to erectile tissue. Br J Urol. 1981; 53:42-6.
- Orvis BR, McAninch JW: Penile rupture. Urol Clin North Am. 1989; 16:369-75.
- Uygur MC, Gulerkaya B, Altug U, Germiyanoglu C, Erol D: 13 years experience of penile fracture. Scand J Urol Nephrol. 1997; 31:265-6.
- Babu N: Rupture of the dorsal vein mimicking fracture of the penis. BJU Int. 1999; 84:179-80.
- Ozen HA, Erkan I, Alkibay T, Kendi S, Remzi D: Fracture of the penis and long-term results of surgical treatment. Br J Urol. 1986; 58:551-2.
- Mellinger BC, Douenias R: New surgical approach for operative management of penile fracture and penetrations trauma. Urology 1992; 39:429-32.
- Seftel AD, Haas CA, Vafa A, Brown SL: Inguinal scrotal incision for penile fracture. J Urol. 1998; 159:182-4.
_____________________
Received: August 8, 2002
Accepted after revision: February 4, 2003
________________________
Correspondence address:
Dr. Luciano Alves Favorito
Rua Professor Gabizo, 104 / 201
Rio de Janeiro, RJ, 20271-320, Brazil
Fax: + 55 21 3872-8802
E-mail: favorito@uerj.br