STEREOLOGICAL
STUDY OF COLLAGEN AND ELASTIC SYSTEM IN THE DETRUSOR MUSCLE OF BLADDERS
FROM CONTROLS AND PATIENTS WITH INFRAVESICAL OBSTRUCTION
(
Download pdf )
MAURICIO RUBINSTEIN, FRANCISCO J. SAMPAIO, WALDEMAR S. COSTA
Urogenital Research Unit, State University of Rio de Janeiro, Rio de Janeiro, Brazil
ABSTRACT
Objective:
Compare detrusor muscle of normal and patients with infravesical obstruction,
quantifying the collagen and elastic system fibers.
Materials and Methods: We studied samples
taken from bladders of 10 patients whose ages ranged from 45 to 75 years
(mean = 60 years), who underwent transvesical prostatectomy for treatment
of BPH. Control material was composed of 10 vesical specimens, removed
during autopsies performed in cadavers of accident victims, with ages
between 18 and 35 years (mean = 26 years).
Results: The results of collagen and elastic
fibers quantification (volumetric density) demonstrated the following
results in percentage (mean +/- standard deviation): collagen in BPH patients
= 4.89 +/- 2.64 and 2.32 +/- 1.25 in controls (p < 0.0001), elastin
in BPH patients = 10.63% +/- 2.00 and 8.94% +/- 1.19 in controls (p <
0.0001).
Conclusion: We found that the components
of connective tissue, collagen and elastic system fibers are increased
in the detrusor muscle of patients with infravesical obstruction, when
compared to controls.
Key
words: bladder, prostatic hyperplasia, bladder outlet obstruction,
collagen, elastin
Int Braz J Urol. 2007; 33: 33-41
INTRODUCTION
The
benign prostatic hyperplasia (BPH) is a pathologic process that contributes
but is not the only cause of lower urinary tract symptoms in men. It is
recognized today that part of the symptoms in men with BPH may be the
result of a detrusor muscle dysfunction related to age (1).
In patients with bladder outlet obstruction
(BOO), in addition to hypertrophic changes in smooth musculature, other
changes related to the collagen and to the elastic system fibers were
already evidenced. However, most of theses studies were conducted on animals
(2-4).
Kondo & Susset (2) did not verify changes
in collagen in bladders of dogs subjected to infravesical obstruction.
On the other hand, an increase in the amount of collagen was described
by Dixon et al. (4) in bladders of swine subjected to partial urethral
obstruction.
Uvelius & Mattiasson (3) described in
rats, the decrease in the amount of collagen in detrusor muscle hypertrophy
caused by infravesical obstruction.
Nielsen et al (5) subjected 9 pigs to chronic
partial infravesical obstruction through an urethral ring. The results
showed an 8-fold increase in total collagen and in type I and III collagen.
Collagen and elastic fibers are the main
components of extracellular matrix; they are present in the bladder wall
and are closely related to vesical compliance (6). The increase of collagen
and other components of extracellular matrix occur as a tissue response
to injury and can lead to fibrosis of the organ. Previous studies have
demonstrated that collagen synthesis is increased in pulmonary fibrosis
(7), in glomerulosclerosis (8) and in other pathologies.
Congenital or acquired infravesical obstruction
can result in a fibrotic vesical wall, characterized by trabeculation,
increase of connective tissue, low volumetric capacity under high pressures
and, in some cases, the occurrence of non-inhibited contraction of detrusor
muscle. The vesical wall can accumulate connective tissue and evolve to
a fibrotic process in consequence of a neurologic (myelomeningocele, spinal
cord lesion) or obstructive (BPH) process. Such pathological conditions
can result in low capacity, high pressure and low vesical compliance (9).
This study aims to compare bladders of normal
patients and those with infravesical obstruction, quantifying by stereological
and computer-assisted methods the collagen and elastic system fibers of
detrusor muscle.
MATERIALS AND METHODS
We
studied samples with approximately 2 x 2 cm, including all the layers
of vesical dome, taken from bladders of 10 patients whose ages ranged
from 45 to 75 years (mean = 60 years), who underwent transvesical prostatectomy
for treatment of BPH. The prostatic mass removed weighted 95 ±
10 grams in average. Previously to surgery, all patients were subjected
to an urodynamic study in order to confirm and characterize the presence
of BOO. A detrusor pressure above 100 cm of H2O and an urinary
flow lower than 10 ml/s were considered as urodynamic evidence of BOO.
The methodology and definitions used in the work complied with the International
Continence Society standards (10). All patients who presented vesical
instability on the urodynamic examination were excluded from the study.
In all cases an informed consent was obtained with the patient for removal
of vesical samples.
Control material was composed of 10 vesical
specimens, removed during autopsies performed in cadavers of accident
victims, with ages between 18 and 35 years (mean = 26 years). The autopsy
was performed up to 6 hours after death, and it was verified that there
was no compromise of urogenital system organs. The removed fragments included
all layers of vesical dome and measured about 2 x 2 cm. The study protocol
was approved by the Committee on Human Research of the State University
of Rio de Janeiro.
Immediately after the removal, the material
was fixed in buffered formalin 10% (pH = 7.2) during 48 to 72 hours, and
subsequently underwent a routine histological processing for inclusion
in paraffin. The resultant blocks were then subjected to serial sections
of 5-µm thickness, obtaining 10 sections from each bladder fragment.
Sections were stained by Picro-Sirius Red
technique for evidencing collagen and by Weigert’s Fuchsin-Resorcin
for characterizing the elastic system fibers.
Image acquisition and analysis - Five sections
were randomly analyzed, from each bladder, and in each section, 5 fields
were analyzed, totaling 15 fields per bladder.
Quantification of the elastic system was
made with sections stained by Weigert’s Fuchsin-Resorcin. The analyzed
fields were digitized to a final magnification of x400 using a video camera
coupled to a light microscope. The alleatory histological areas were quantified
using a M-42 test-grid system on the digitized fields on the screen of
a color monitor. The stereological method has been described in detail
elsewhere (11,12).
For quantification of collagen fibers the
sections stained by Picro-Sirius Red technique were observed under polarized
light (13). The analyzed images were obtained with a magnification of
x400 using a video camera coupled to a light microscope.
The stereological parameter employed for
estimating the contents of extracellular matrix (collagen and elastic
system fibers) was volumetric density (Vv). Mean values of Vv were calculated
for both groups in relation to elastic fibers and collagen and subsequently
compared.
Data were analyzed on Graphpad InStat software
(Graphpad). Mann-Whitney test was used for analysis of results, considering
a value of p < 0.05 as significant.
RESULTS
The
observation of histological sections showed an increase of collagen and
elastic system fibers in the detrusor muscle of patients with infravesical
obstruction, compared to the controls (Figure-1).

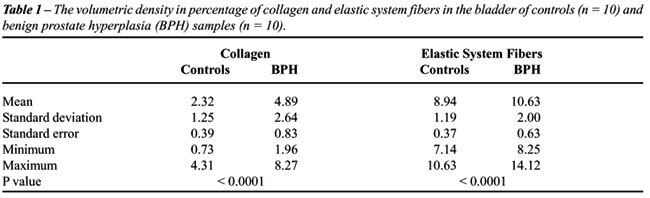
The results of quantification of collagen
and elastic system fibers are presented on Table-1.
DISCUSSION
The
morphology of normal human bladder has been studied and compared to the
obstructed bladder and to the elderly bladder through optic and electronic
microscopy (6,14). In the bladder of patients without urologic disease,
muscle fibers are grouped with few connective tissue between their bundles.
In the obstructed bladder, however, many muscle fibers are surrounded
by connective tissue bundles, and they also change their function, becoming
involved in collagen synthesis (15).
Kim et al (16) analyzed in rats the effects
of partial obstruction of bladder over type I and III collagen, and the
relationship between detrusor contractility and types of collagen. The
results showed an increase in total collagen following infravesical obstruction
and a decrease following the obstruction’s relief. This work suggests
that a change in localization and quantity of collagen leads to vesical
alterations, which can impair detrusor contractility. In our work, conducted
in humans and employing a different methodology, confirms the findings
by Kim et al. (16), demonstrating a significant increase not only in collagen
but also of elastic system fibers in patients with vesical obstruction.
Cortivo et al. (6) evaluated the connective
tissue of bladders of normal patients and patients with infravesical obstruction.
Three distinct groups were assessed: 1) 3-month children with infravesical
obstruction, 2) children between 4 to 8 years with partial infravesical
obstruction and 3) adults with chronic infravesical obstruction. An increase
of elastic tissue occurred in newborns and in adults with obstruction.
Collagen did not present any changes between the groups under study. In
this work, according to the authors, collagen and elastic fibers were
not quantified. In our current study an important increase of elastic
tissue was observed, corroborating, partially, the results from Cortivo
et al. (6), however, differently from their work (6), our results demonstrated
a significant increase of collagen in the detrusor muscle of patients
with obstructive BPH.
Gosling & Dixon (17) compared microscopic
findings from biopsies of the detrusor muscle with the grade of vesical
trabeculation assessed by cystoscopy. The author observed an important
infiltration of connective tissue elements in the detrusor muscle of patients
with severely trabeculated bladders. Data from our current work, also
show that collagen surrounds and infiltrates the muscle bundles, suggesting
that fibrous elements can lead to a reduction of compliance in bladders
of patients with infravesical obstruction.
Gilpin et al. (9) while studying the morphology
and morphometry of detrusor muscle fibers from patients with obstruction,
described structural changes of the vesical wall, represented by collagen
deposit in muscular interstice, and by the increase in volume of muscle
fibers, what is in accordance to our results.
Freedman et al. (18) demonstrated that the
relationship between smooth muscle versus connective tissue remained the
same in control (normal) and obstructed fetal bladders. These findings
show that the amount of collagen associated with infravesical obstruction
is also a controversial subject in human bladders.
Lepor et al. (19), with the purpose of characterizing
the effects of aging and of obstructive BPH over the vesical wall, conducted
a retrospective study in 86 vesical samples, obtained from medical files,
and removed during autopsies. The study was divided into 4 groups: 1)
men aged between 35 and 45 years; 2) men aged between 65 and 75 years;
3) women aged between 35 and 45 years; and 4) women aged between 65 and
75 years. The groups were divided in order to select men with BPH and
without BPH. There was a significant increase of density in the smooth
muscle and connective tissue area in group 1 vs. group 2 (2.90 +/- 0.22
vs. 2.33 +/- 0.16) and in group 3 vs. group 4 (2.85 +/- 0.13 vs. 2.03
+/- 0.20). The increase in the connective tissue ratio was age-dependent
in both female and male groups. Based on these results, the authors suggest
that aging, and not BPH, is related to an increase of fibrosis in the
detrusor muscle. Nevertheless, one must take into account that the examined
material in this study came from patients who did not undergo urodynamic
tests, that would confirm or not the presence of infravesical obstruction.
In our study, the previous conduction of an urodynamic assessment confirmed
the existence of an obstructive process in all the patients under study.
Our results showed that there was a significant increase of collagen and
elastic fibers when the groups of men with BPH and without BPH were compared.
The study by Holm et al. (20) questions
if the fibrosis of the detrusor muscle is a consequence of infravesical
obstruction, of the patient’s age, or both factors. Morphological
studies of vesical wall were performed through biopsies from young patients
without disease, patients with infravesical obstruction, and elderly without
obstruction. It was observed fibrosis inside and around the muscle fascicles,
in the same proportion in obstructed patients and in elderly. The results
from this work pose the question whether the fibrotic changes of detrusor
muscle occur due to obstruction itself, to aging, or both.
Gosling (15) demonstrated that in the elderly,
the bladder differs from the obstructed bladder regarding the collagen
deposit. In the elderly bladder there is no evidence of collagen synthesis
by smooth muscle fibers. On the other hand, in the bladder that is obstructed
by BPH there is an accumulation of connective tissue in the detrusor muscle,
where several smooth muscle fibers change their function, and become more
involved with the collagen synthesis. Thus, the author concluded that
it is unlikely that the changes occurring in the bladder of patients with
obstruction merely reflect alteration due to aging. The results of the
current work ratify these data (15), objectively demonstrating that, in
the bladder obstructed by BPH, there is an accumulation of connective
tissue in the detrusor muscle.
Deveaud et al. (21) analyzed 45 children
who underwent surgical treatment for non-compliant and fibrotic bladders
due to a number of causes (myelomeningocele, posterior urethral valve,
vesicoureteral reflux). Vesical fragments were analyzed through immunohistochemical
for localizing collagen. A major infiltration of connective tissue was
evidenced in detrusor’s smooth muscle bundles. The results showed
an increase in total collagen, through dosing of total hydroxyproline
content, and a significant increase in type I and III collagen. The work
suggests that the collagen deposit in the detrusor muscle is a marked
histological characteristic of non-compliant bladders, regardless of their
etiology. Our results show a concordance with this work (21) even though
the methodology and groups under study were different. In our study, even
though a separate quantification of type I and type III collagen was not
performed, the greenish color present in the sections observed under polarization
microscopy is highly expressive and suggests the presence of a significant
amount of type III collagen.
It is important to highlight that the majority
of previous studies, in humans, were conducted without confirmation of
an obstructive condition by urodynamic tests.
Inui et al. (22) observed changes in connective
tissue of the detrusor muscle of patients with obstructive BPH. Thirteen
normal men with ages ranging from 25 to 90 years (68.5 +/- 18) and 26
cases of BPH patients with ages between 60 and 94 years (71.6 +/- 9.2)
were studied. BPH diagnosis was made based on the prostate transrectal
ultrasonography. The mean values for connective tissue and smooth muscle
between control and BPH cases were subsequently compared through computer
assisted color image analysis. The authors found that abnormal increase
of connective tissue in addition to smooth muscle hypertrophy and/or hyperplasia
could contribute to advanced bladder hypertrophy caused by infravesical
obstruction. Our findings confirm the increase of connective tissue in
patients with BPH and demonstrate a significant difference in the percentage
of collagen and elastic system fibers between the control and BPH groups.
Recently, Collado et al. (23) studied by
computer assisted morphometry the detrusor muscle cell diameter and the
connective tissue-to-smooth muscle ratio in patients with bladder outlet
obstruction, acute urinary retention and a nonobstructed control group.
The author found morphometric differences in detrusor muscle cell diameter
and the connective tissue-to-smooth muscle ratio between controls and
patients with obstruction. Also, it was found an increase in detrusor
muscle cell diameter and fibrosis in bladder outlet obstruction, which
are in agreement with our findings concerning extracellular matrix components.
The understanding of changes consequent
to a response to vesical injury, may allow the development of strategies
to prevent the pathologic remodeling of extracellular matrix observed
in diseased bladders. Obstructive processes, diseases related to age,
or even aging itself, can influence vesical function. The relationship
between obstruction and aging has not been completely clarified. The lower
urinary tract symptoms are not specific, and alone they do not enable
the diagnosis of obstruction. The symptomatology in certain conditions,
such as vesical instability and detrusor hypocontractility without obstruction,
mimic those of obstructive BPH, but there is no proof that such conditions
result solely from aging.
Even if we know that some changes occurring
in the bladder that is subjected to infravesical obstruction are possibly
related to aging processes, a comparison with bladders of normal young
individuals, such as the one we performed on this work, can be useful
for establishing a pattern of the different vesical components, which
will be modified either by aging or by pathologic processes.
In conclusion, we found that the components
of connective tissue, collagen and elastic system fibers are increased
in the detrusor muscle of patients with infravesical obstruction.
ACKNOWLEDGMENTS
Supported by grants from the National Council of Scientific and Technological Development (CNPq), and Foundation for Research Support of Rio de Janeiro (FAPERJ).
CONFLICT OF INTEREST
None declared.
REFERENCES
- Elbadawi A: Functional anatomy of the organs of micturition. Urol Clin North Am 1996; 23: 177-210.
- Kondo A, Susset JG: Collagen content in detrusor muscle and ratio of bladder weight to body weight. Acta Urol Jap 1973; 19: 683-686.
- Uvelius B, Mattiasson A: Collagen content in the rat urinary bladder subjected to infravesical outflow obstruction. J Urol 1984; 132: 587-590.
- Dixon JS, Gilpin CJ, Gilpin SA, Gosling JA, Brading AF, Speakman MJ: Sequential morphological changes in the pig detrusor in responses to chronic partial urethral obstruction. Br J Urol 1989; 64: 385-390.
- Nielsen KK, Andersen CB, Petersen LK, Oxlund H, Nordling J: Morphological, stereological, and biochemical analysis of the mini-pig urinary bladder after chronic outflow obstruction and after recovery from obstruction. Neurourol Urodyn. 1995; 14: 269-284.
- Cortivo R, Pagano F, Passerini G, Abatangelo G, Castellani I: Elastin and collagen in the normal and obstructed urinary bladder. Br J Urol 1981; 53: 134-137.
- Kuhn C, Boldt J, King T, Crouch E, Vartio T, Mcdonald J: An immunohistochemical study of architectural remodeling and connective tissue synthesis in pulmonary fibrosis. Am Rev Respir Dis 1989; 140: 1693-1703.
- Peten E, Striker L, Carome M, Elliott S, Yang CW, Striker G: The contribution of increased collagen synthesis to human glomerulosclerosis: A quantitative analysis of a2IV collagen mRNA expression by competitive polymerase chain reaction. J Exp Med 1992, 176: 1571-1576.
- Gilpin S, Gosling J, Barnard R: Morphological and morphometric studies of the human obstructed, trabeculated urinary bladder. Br J Urol 1985; 57: 525-529.
- Abrams P, Blaivas JG, Stanton SL, Andersen JT: The standardization of terminology of lower urinary tract function. Scand J Urol Nephrol 1988; 14 (Suppl): 5-19.
- Pinheiro AC, Costa WS, Cardoso LE, Sampaio FJ: Organization and relative content of smooth muscle cells, collagen and elastic fibers in the corpus cavernosum of rat penis. J Urol 2000; 164: 1802-1806.
- Weibel ER, Kistler GS, Scherle WF: Practical stereological methods for morphometric cytology. J Cell Biol 1966; 30: 23-38.
- Junqueira LCU, Montes GS, Sanchez EM: The influence of tissue section thickness on the study of collagen by the Picrosirius-polarization method. Histochemistry 1982; 74: 153-156.
- Mayo ME, Lloyd-Davies RW, Shuttleworth KED, Tighe JR: The damaged human detrusor: functional and electron microscopic changes in disease. Br J Urol 1973; 45: 116-125.
- Gosling JA: Modification of bladder structure in response to outflow obstruction and ageing. Eur Urol 1997; 32 (suppl 1): 9-14.
- Kim JC, Yoon JY, Seo SI, Hwang TK, Park YH: Effects of partial outlet obstruction and its relief on types I and III collagen and detrusor contractility in the rat. Neurourol Urodyn 2000; 19: 29-42.
- Gosling JA, Dixon JS: Detrusor morphology in relation to bladder outflow obstruction and instability. In Hinman FJr., editor. Benigh prostatic hypertrophy. New York, Springer. 1983, pp 666-671.
- Freedman AL,Qureshi F, Shapiro E, Lepor H, Jacques SM, Evans MI, Smith CA, Gonzalez R, Johnson MP: Smooth muscle development in the obstructed fetal bladder. Urology 1997; 49: 104-107.
- Lepor H, Sunaryadi I, Hartanto V, Shapiro E: Quantitative morphometry of the adult human bladder. J Urol 1992; 148: 414-417.
- Holm NR, Horn T, Hald T: Bladder wall morphology in ageing and obstruction. Scand J Urol Nephrol 1995; 29: 45-49.
- Deveaud CM, Macarak EJ, Kucich U, Ewalt DH, Abrams WR, Howard PS: Molecular analysis of collagens in bladder fibrosis. J Urol 1998; 160: 1518-1527.
- Inui E, Ochiai A, Nasa Y, Ukimura O, Kojima M: Comparative morphometric study of bladder detrusor between patients with benigh prostatic hyperplasia and controls. J Urol 1999; 161: 827-830.
- Collado A, Batista E, Gelabert-Mas A, Corominas JM, Arano P, Villavicencio H: Detrusor quantitative morphometry in obstructed males and controls. J Urol. 2006; 176: 2722-8.
____________________
Accepted after revision:
September 14, 2006
_______________________
Correspondence address:
Waldemar S. Costa
Urogenital Research Unit - UERJ
Av. 28 de Setembro, 87 – fundos – FCM – terreo
20551-030, Rio de Janeiro, RJ, Brazil
Fax: + 55 21 2587-6121
E-mail: wscosta@gmail.com
Bladder
outlet obstruction produces histological changes in the detrusor, including
an increased collagen concentration in adult and fetal bladders (1-4).
The authors of this paper have corroborated that the components of connective
tissue are increased in the detrusor muscle of patients with infravesical
obstruction. While this is not the first study regarding the association
between bladder wall collagen deposition and bladder outlet obstruction,
it is one of the first report to demonstrate a clear demarcation in collagen
content and elastic systems fiber of the obstructed and unobstructed adult
human male bladder. This study may enable us to better understand the
human bladder reaction to bladder outlet obstruction. Studies of this
type should be encouraged.
However,
much more work needs to be done to establish a link between lower urinary
tract symptoms and this histological finding. First, although they stated
that the greenish color present in the sections observed under polarization
microscopy suggests the presence of a significant amount of type III collagen,
a separate quantification of type I and type III collagen was not performed
and no analysis of collagen content by symptom type was reported. Second,
no mention was made of compliance measurements. This is of potential since
patients with a low compliant bladder expect to have a significant increase
in connective tissue compared to those without a low compliant bladder
(5). It would have certainly been useful to determine what level of bladder
wall collagen is associated with detectable changes in bladder compliance.
This work would add to the growing body of evidence linking specific changes
in detrusor structure or function with lower urinary tract symptoms. Finally,
the increase in the connective tissue may be age-dependent (4). Thus,
it would be better to include elderly patients without bladder outlet
obstruction in the study.
REFERENCES
- Susset JG, Servot-Viguier D, Many F, Madernas P, Black R: Collagen in 155 human bladders. Invest Urol. 1978; 16: 204-6.
- Uvelius B, Mattiasson A: Collagen content in the rat urinary bladder subjected to infravesical outflow obstruction. J Urol. 1984; 132: 587-90.
- Kim KM, Kogan BA, Massad CA, Huang YC: Collagen and elastin in the obstructed fetal bladder. J Urol. 1991; 146: 528-31.
- Lepor H, Sunaryadi I, Hartanto V, Shapiro E: Quantitative morphometry of the adult human bladder. J Urol. 1992; 148: 414-7.
- Ohnishi N, Kishima Y, Hashimoto K, Kiwamoto H, Esa A, Sugiyama T, et al.: Morphometric study of low compliant bladder. Hinyokika Kiyo 1994; 40: 657-61.
Dr. Jae-Seung Paick
Department of Urology
Seoul National University Hospital
Seoul, Korea
E-mail: jspaick@snu.ac.kr
EDITORIAL COMMENT
In
our urological practice, it is commonly found that patients with profound
bladder outlet obstruction (BOO) may have a low bladder compliance. The
low compliant bladder contributes to a high intravesical pressure and
endangers upper urinary tract function. Moreover, in the patients with
low bladder compliance, the detrusor contractility is usually inadequate
to completely empty the bladder during micturition. The increased connective
tissue density in the bladder wall may not only constrict the distensibility
of the urinary bladder but also result in low bladder contractility.
In
this article, the authors found the collagen and elastic system fibers
increase in the bladder wall in the patients with urodynamically proven
BOO compared to the bladders in the non obstructed cadavers. Previous
studies have shown in patients with BOO and ageing, the collagen content
increases. The results of this study are compatible with the previous
works using rat models and human bladders and further demonstrate that
the connective tissue components are increased in the bladder wall of
BOO in a group of patients with a mean age of 60 years.
Bladder
“fibrosis” results in trabeculation, reduced capacity, increased
intravesical pressure and suppressed detrusor contractility. This pathological
change of the bladder wall is commonly found in varying diseases including
neurogenic bladder, BOO, ageing and chronic cystitis. The true mechanisms
for the increased connective tissue density in the bladder wall have not
been completely elucidated yet. Recent studies have shown that BOO may
induce increase in nerve growth factor (NGF) production in the suburothelium,
which might result in a cascade of inflammatory reactions, lowering sensory
threshold and remodeling of the micturition pathways (1). The increased
NGF levels in bladder afferent pathways could contribute to the emergence
of bladder overactivity as well as somal hypertrophy and hyperexcitability
of bladder afferent neurons (2). It is interesting to find that in patients
with transient BOO, the bladder compliance will turn to normal after relief
of obstruction, however, in patients with chronic BOO, the changes of
the bladder wall will not. Neural plasticity induced increase of connective
tissue density in the bladder wall after BOO and the factors responsible
for their reversibility deserve further investigations.
REFERENCES
- Steer WB, Tuttle JB: Mechanisms of Disease: the role of nerve growth factor in the pathophysiology of bladder disorders. Nat Clin Pract Urol. 2006; 3: 101-10.
- Yoshimura N, Bennett NE, Hayashi Y, Ogawa T, Nishizawa O, Chancellor MB, et al: Bladder overactivity and hyperexcitability of bladder afferent neurons after intrathecal delivery of nerve growth factor in rats. J Neurosci. 2006; 26: 10847-55.
Dr. Hann-Chorng Kuo
Dept. Urology, Buddhist Tzu Chi General Hospital
Buddhist Tzu Chi University
Hualien, Taiwan
E-mail:hck@tzuchi.com.tw