PREOPERATIVE
VALSAVA LEAK POINT PRESSURE MAY NOT PREDICT OUTCOME OF MID-URETHRAL SLINGS.
ANALYSIS FROM A RANDOMIZED CONTROLLED TRIAL OF RETROPUBIC VERSUS TRANSOBTURATOR
MID-URETHRAL SLINGS
(
Download pdf )
ELISABETTA COSTANTINI, MASSIMO LAZZERI, ANTONELLA GIANNANTONI, VITTORIO BINI, ALBERTO VIANELLO, ERVIN KOCJANCIC, MASSIMO PORENA
Department of Medical and Surgical Specialties and Public Health, Section of Urology and Andrology (EC, ML, AG, AV, MP), and Department Internal Medicine (VB), University of Perugia, Perugia, Italy and Department of Urology (EK), University of Udine, Udine, Italy
ABSTRACT
Objective:
To test the hypothesis that preoperative Valsalva leak point pressure
(VLPP) predicts long-term outcome of mid-urethra slings for female stress
urinary incontinence (SUI).
Materials and Methods: One hundred and forty-five
patients with SUI were prospectively randomized to two mid-urethra sling
treatments: Tension free vaginal tape (TVT) or transobturator tape (TOT).
They were followed-up at 3, 6, 12 months post-operatively and then annually
for the primary outcome variable, i.e. dry or wet and secondary outcome
variables such as scores on the urogenital distress inventory (UDI-6)
and the impact of incontinence on quality of life (IIQ-7) questionnaire
as well as patient satisfaction as scored on a visual analogue scale (VAS).
Preoperative VLPP was correlated with primary and secondary outcome variables.
Results: Mean follow-ups were 32 ±
12 months (range 12-55) for TVT and 31 ± 15 months (range 12-61)
for TOT. When patients were analyzed according to VLPP stratification,
95 (65.5%) patients showed a VLPP > 60 cm H2O and 50 (34.5%)
patients had a VLPP ≤ 60 cm H2O. The overall objective
cure rates were 75.8% for patients with VLPP > 60 cm H2O
and 72% for those with VLPP ≤ 60 cm H2O (p < 0.619).
No significant differences in objective cure rates emerged when patients
were stratified for pre-operative VLPP and matched for TOT or TVT procedures:
VLPP > 60 cm H2O (82 % vs. 68.9% p < 0.172); VLPP ≤
60 cm H2O (68% vs. 76% p < 0.528).
Conclusions: When patients were stratified
for preoperative VLPP (≤ or > of 60 cm H2O), preoperative
VLPP was not linked to outcome after TVT or TOT procedures.
Key
words: urinary incontinence; Valsalva leak point pressure; tension
free vaginal tape; transobturator tape
Int Braz J Urol. 2008; 34: 73-83
INTRODUCTION
Since
the tension-free vaginal tape (TVT) procedure was first described by Ulmsten
et al. in 1996 (1), mid-urethral sling procedures have been established
as safe and effective in the treatment of female stress urinary incontinence
(SUI) (2). Long-term follow-ups showed high cure rates ranging from 81%
to 95% for TVT and the recently introduced tension free transobturator
tape (TOT) procedures (3 - 6). Although most studies analyzed the safety
and the efficacy of mid-urethra slings, outcomes, and the complication
rate, a few tried to address the issue of factors predicting long-term
outcome.
Urethral integrity was first investigated
as outcome predictor in patients who underwent mid urethral sling operations
for SUI. Miller et al. found at 3 months after surgery that TOT was nearly
6 times more likely to fail than TVT in subjects with a preoperative maximum
urethral closure pressure at or below 42 cm H2O (7). The Valsalva
Leak Point Pressure (VLPP), which the International Continence Society
(ICS) defined as the intravesical pressure at which urine leakage occurs
due to increased abdominal pressure generated by a Valsalva maneuver,
is considered an objective parameter for SUI severity (8). In 1993, McGuire
et al. demonstrated that leakage pressure during the Valsalva maneuver
was a reliable method for assessing the urethral sphincter mechanism (9).
These findings were confirmed by Feldner Jr. et al. and Albo et al. (10,
11), and indeed Albo et al. concluded that the VLPP might be a good measure
of urethral sphincter dysfunction even though it was not associated with
symptom severity, quantity of urine loss, or its effect on the patient’s
Quality of Life (QoL).
Patients with a low VLPP on preoperative
urodynamic assessment were reported to have increased risk of treatment
failure (12, 13). In a recent investigation into preoperative VLPP as
a predictor of outcome after distal urethral sling procedures, Rodriguez
et al. reported the VLPP was useful for diagnosing SUI, but, at a 14-month
follow-up, appeared to be of minimal importance in predicting outcome
(14). On the other hand, in patients who underwent mid-urethra slings,
O’Connor reported excellent results in patients with a VLPP >
60 cm H2O but not in those with a low VLPP (≤ 60 cm H2O)
(15). As both these studies had short follow-ups and did not match outcomes
for different types of surgery, the role of VLPP in predicting the risk
of failure at long-term follow-up remains an open issue.
The present study investigated the prognostic
value of VLPP for mid-urethral sling outcomes using data from a randomized
controlled study of 145 women with stress or mixed urinary incontinence
that were treated with either TVT or TOT (16).
MATERIALS AND METHODS
From
May 2002 to November 2005, 145 patients affected by SUI as defined by
ICS (8) and who were candidates for the mid-urethral sling procedure were
prospectively randomized by a predetermined computer-generated randomization
code, to the retropubic approach (TVT) or the transobturator route (TOT).
Randomization was done using sealed, opaque, numbered envelopes, which
contained the randomized allocation. The Regional Ethics Committee approved
the study protocol and all patients gave written informed consent.
Inclusion criteria were stress or mixed
urinary incontinence defined according to ICS guidelines and associated
with urethral hypermobility. Hypermobility was defined as a Q-tip test
> 30° (our cut-off). Exclusion criteria were > grade II prolapse
in any vaginal compartment, previous incontinence surgery, urine retention,
neurogenic bladder and psychiatric disorders. The pre-operative work-up
included a detailed case history, clinical, neurological and urogynecological
examination using the Half-Way system (17), the POP-Q system classification
(18), and a pelvic static ultrasound scan. All patients underwent a stress
test in the supine position at physiological maximum bladder capacity.
Urethral hypermobility was evaluated not only by the Q-tip test but also
by perineal ultrasound, which is routinely performed at our Institution.
During the scan the distance was measured between the bladder neck and
a line at right angles to the pubic bone plane. A cut-off value > 7
was indicative of a hypermobile urethra (19). Urinary incontinence was
classified as recommended by the International Consultation on Incontinence
and graded according to the Ingelman Sunderberg classification (20). All
patients completed two validated questionnaires on quality of life, i.e.
the Urogenital Distress Inventory (UDI-6) and the Impact Incontinence
Quality of life (IIQ-7) before surgery, at 3, 6, 12 months postoperatively
and then annually. Patient satisfaction was scored by inviting patients
to mark the grade of satisfaction on a VAS scale from 0-10, on which 10
was maximum satisfaction and zero no satisfaction. Before surgery patients
performed a 1-h pad test and completed a bladder diary for three days.
All patients underwent a preoperative urodynamic
assessment, which included uroflowmetry, provocative cystometry and urethral
profilometry. In accordance with ICS guidelines, filling cystometry was
performed in all patients with saline solution at a flow rate of 25 mL/min
by a double lumen 8F catheter (one lumen was used to fill the bladder
while the other lumen was connected to a pressure transducer to measure
intravesical pressure); a balloon catheter was placed in the rectum to
record abdominal pressure. The VLPP was determined at a bladder volume
of 200 mL. Patients were instructed to perform several Valsalva maneuvers
with a gradual increase in abdominal pressure and urine leakage was recorded
as previously described (21). Patients were stratified by VLPP > 60
cm H2O or VLPP ≤ 60 cm H2O.
Standard operating techniques were, respectively,
the Ulmsten (1) (TVT® - Ethicon) and Delorme techniques (5); no concomitant
procedure was performed. The trans-obturator tape was a fusion-welded,
non-woven, non-knitted polypropylene tape (Obtape® Mentor-Porges).
No preoperative choice between general and regional anesthesia was made.
In both procedures, a Foley catheter was always inserted for 24 hours.
After the catheter was removed, if post-void residual volume was more
than 50% of bladder volume, intermittent catheterization was proposed.
The surgeons were blinded to preoperative VLPP results.
The primary outcome variable was continence
status: dry or wet as deduced by clinical examination, stress test and
patient interview. Patients were classified in two categories: dry (no
leakage during clinical examination and/or stress test and/or reported
by patients) vs. wet. Wet patients were then sub-divided into “improved”
(more than 50% reduction in incontinence episodes) or “failure”.
Secondary outcome variables were scores on the quality of life questionnaires
and the VAS scale.
Patients were followed-up at 3, 6, 12 months
post-operatively and then annually, and at each check-up a blinded assessor
measured primary and secondary outcome variables. Terminology followed
ICS guideline (8).
VLPP was analyzed retrospectively using
data from a randomized controlled study (16) which was accordingly powered.
The Mann-Whitney test compared ordinal and non-normally distributed continuous
variables. Deviations from Gaussian distribution were checked using the
Kolgomorov-Smirnov test with the Lilliefors method. Categorical data were
analyzed by the chi-square test or Fisher’s exact test, as appropriate.
The level of statistic significance was set at P < 0.05. All calculations
were carried out with SPSS release 13.0, SPSS Inc., Chicago, USA, 2004.
RESULTS
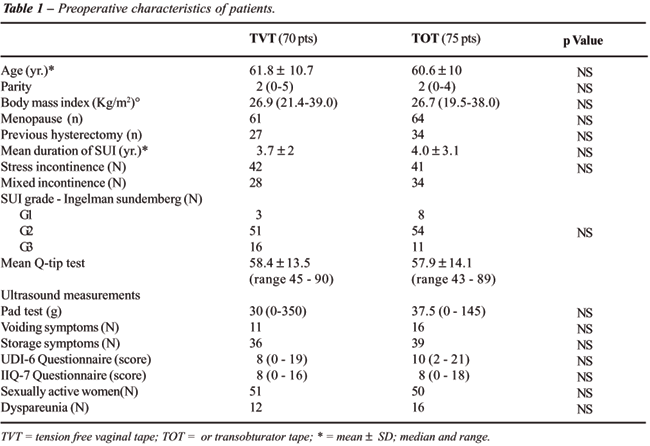
Table-1
shows the two groups (TVT vs. TOT) were well balanced demographically.
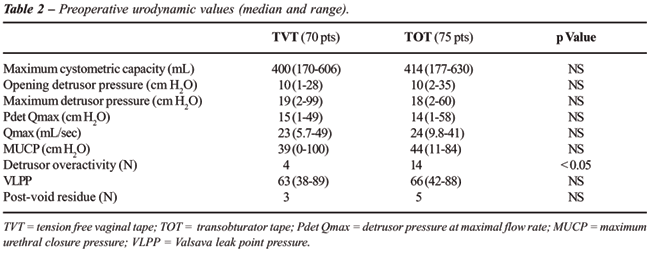
No patient was lost during follow-up. Preoperative urodynamic parameters
were similar in the two groups, except for detrusor overactivity, which
was more frequent in patients who received TOT (Table-2).
The overall median follow-up was 35 months
with a mean follow-up of 32 ± 12 months (range 12 - 55) for the
TVT group and 31 ± 15 months (range 12 - 61) for the TOT procedure.
110 patients (75.9%) had a follow-up ≥ 24 months. Table-3 summarizes
the operating data. The overall objective cure rates (dry) were 71.4%
for TVT and 77.3% for TOT. When dry patients were grouped with the “wet
but improved” the success rates rose to 90% and to 90.6% respectively.

VLPP was > 60 cm H2O in 95/145
patients (65.5%). TOT was performed in 50 of these 95 patients (52.6%),
and in 25/50 patients (50%) with VLPP £ 60 cm H2O. TVT
was performed in the others: 45 patients (47.4%) with a VLPP > 60 cm
H2O and 25/50 patients (50%) with VLPP ≤ 60 cm H2O.
The overall objective cure rates were 75.8% for patients with VLPP >
60 cm H2O and 72% in patients with VLPP ≤ 60 cm H2O
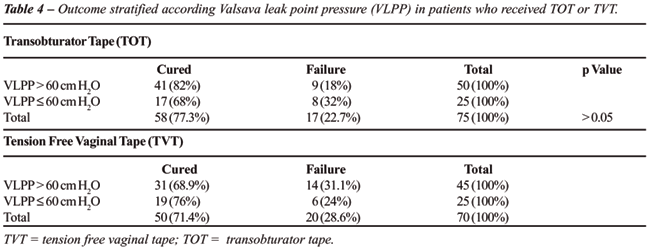
(p < 0.619). No significant differences emerged in objective cure rates
when VLPP-stratified patients were matched for TOT or TVT procedures (VLPP
> 60 cm H2O: 82 % TOT vs. 68.9% TVT; p < 0.172; VLPP
≤ 60 cm H2O: 68% TOT vs. 76% TVT p < 0.528). Data
are shown in Table-4. Table-5 reports outcomes in patients with mixed
incontinence. No significant difference was observed.

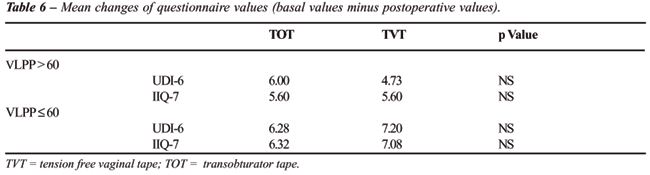
Postoperative changes in questionnaire scores
were not significant (p > 0.05) when patients were stratified for VLPP
and type of procedure. In patients with VLPP > 60 cm H2O,
the mean post-operative scores were 2.24 for TOT and 2.56 for TVT (UDI-6)
and 1.94 for TOT and 1.93 for TVT (IIQ-7). In patients with VLPP ≤
60 cm H2O, the mean postoperative scores were 2.08 for TOT
and 1.36 for TVT (UDI-6) and 1.72 for TOT and 1.52 for TVT (IIQ-7). Table-6
reports mean changes of the questionnaire values. All questionnaire scores
were significantly lower than the preoperative value reported in Table
1 (p = 0.001). Mean post-operative VAS scores were 8.68 for TOT and 8.24
for TVT in patients with VLPP > 60 cm H2O and 7.88 for TOT
and 8.44 for TVT in patients with VLPP ≤ 60 cm H2O (p
= NS).
COMMENTS
The
present study seems to indicate preoperative VLPP has no bearing on outcomes
after mid-urethral slings as treatment of SUI because when patients were
stratified for pre-operative VLPP values we found no difference in cure
rates, independently of whether TOT or TVT was used as a treatment or
not.
Several authors who used the VLPP to choose
treatment in patients with SUI suggested it might provide prognostic information
(12 - 15, 22, 23). For example, in a series of 43 patients with SUI, O’Connor
et al. (15) reported 77% of patients with a preoperative VLPP > 60
were cured compared with 25% of patients with VLPP ≤ 60 cm H2O.
Rodriguez et al., evaluated 174 patients who underwent distal-urethral
sling procedures, dividing them into four groups according to VLPP values
(group 1: no leakage; group 2: VLPP > 80 cm H2O group 3:
VLPP from 30 to 80; group 4: VLPP < 30). Regardless of the VLPP, overall
objective cure rates were similar in all groups (95%, 92%, 93% and 92%
respectively) as were patient-reported outcomes and the number of daily
pads, even though patients with low VLPP had used more pads per day before
surgery (14). These results were confirmed by Cetinel et al. in an investigation
into seventy-five consecutive patients with urodynamically proven SUI
who underwent TVT (24). When stratified according to preoperative VLPP,
36 patients (48%) had ≤ 60 cm H2O and 39 patients (52%)
had > 60 cm H2O. When cure rates were compared with preoperative
VLPP, no significant difference emerged at a mean follow-up of 21.6 months
(89.7% vs. 88.9% respectively). Abdel-Hady investigated the efficacy of
tension-free vaginal tape (TVT) in 80 women with a low VLPP (≤ 60
cm H2O) in a series of 658 patients (25) and reported an 86%
cure rate (dry) and a 14% improved rate (wet but improved) at 6 months,
concluding that the high efficacy of TVT makes it the first choice treatment
for women with SUI – including those with low VLPP.
Although the findings in the present study
concur with several reports, one weakness in our study design is the mix
of TVT and TOT that could have partly biased results as TOT seems more
suitable than retropubic TVT for SUI with urethral hypermobility (26).
Secondly, dividing patients arbitrarily into two groups on the basis of
a VLPP cut-off of 60 cm H2O may have been a bias. Recently Guerette et
al. found that the cut-off values of VLPP > 60 cm H2O and Maximum Urethral
Closure Pressure > 40 cm H2O were the most predictive factors
of surgical success, showing a sensitivity of 83% and specificity of 79%
(27).
Although most surgeons recognize that outcome
assessment tools are often debatable, the issue assumes marked significance
after operations that are designed to decrease the impact of specific
signs and symptoms such as incontinence, and outcomes are correlated with
preoperative outcome predictors at urodynamics. In the present study we
tried to address issues related to outcome after mid-urethra sling placement
and validation of VLPP as an objective parameter for assessing outlet
region function using established, generally accepted criteria. However,
increasing evidence suggests with urodynamic findings that the patient’s
condition and specific quality of life could be dissociated (28). Although
studies reporting urinary incontinence as outcome and analyzing outcome
predicting factors can never develop the level of evidence seen for other
symptoms or disease states such as oncologic outcome reporting, investigating
pre-operative predictive factors remains mandatory so as to avoid overuse
or misuse of mid-urethra slings and improve quality of care. Minimal requirements
for predictor reporting include not only preoperative VLPP as in our case,
but also peri-operative complications, hospital stays and length of follow-up
data, which seems insufficient in many studies. The 3-year follow-up,
which is presented here, may be a step forward in this direction. Finally,
we cannot forget the individual’s response to surgery for SUI and
the impact that other variables have on single outcome criterion, which
make it difficult to discuss the pathophysiological significance of the
VLPP.
CONCLUSION
Preoperative VLPP, which was stratified for preoperative VLPP (≤ or > of 60 cm H2O), was not dependent on outcome after TVT or TOT. Further studies remain mandatory to confirm these data and to investigate other outcome independent variables.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Ulmsten U, Henriksson L, Johnson P, Varhos G: An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 1996; 7: 81-5; discussion 85-6.
- Rezapour M, Ulmsten U: Tension-Free vaginal tape (TVT) in women with recurrent stress urinary incontinence—a long-term follow up. Int Urogynecol J Pelvic Floor Dysfunct. 2001; 12 (Suppl 2): S9-11.
- Nilsson CG, Falconer C, Rezapour M: Seven-year follow-up of the tension-free vaginal tape procedure for treatment of urinary incontinence. Obstet Gynecol. 2004; 104: 1259-62.
- Jomaa MA: seven-year follow up of tension free vaginal tape (TVT) for surgical treatment of female stress urinary incontinence under local anaesthesia [abstract]. Int Urogynecol J 2003, 14: S69.
- Delorme E: Transobturator urethral suspension: mini-invasive procedure in the treatment of stress urinary incontinence in women. Prog Urol. 2001; 11: 1306-13.
- deTayrac R, Deffieux X, Droupy S, Chauveaud-Lambling A, Calvanèse-Benamour L, Fernandez H: A prospective randomized trial comparing tension-free vaginal tape and transobturator suburethral tape for surgical treatment of stress urinary incontinence. Am J Obstet Gynecol. 2004; 190: 602-8. Retraction in: Am J Obstet Gynecol. 2005; 192: 339.
- Miller JJ, Botros SM, Akl MN, Aschkenazi SO, Beaumont JL, Goldberg RP, et al.: Is transobturator tape as effective as tension-free vaginal tape in patients with borderline maximum urethral closure pressure? Am J Obstet Gynecol. 2006; 195: 1799-804.
- Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al.: The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn. 2002; 21: 167-78.
- McGuire EJ, Fitzpatrick CC, Wan J, Bloom D, Sanvordenker J, Ritchey M, et al.: Clinical assessment of urethral sphincter function.J Urol. 1993; 150: 1452-4.
- Feldner PC Jr, Bezerra LR, de Castro RA, Sartori MG, Baracat EC, de Lima GR, et al.: Correlation between valsalva leak point pressure and maximal urethral closure pressure in women with stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2004; 15: 194-7.
- Albo M, Wruck L, Baker J, Brubaker L, Chai T, Dandreo KJ, et al.: The relationships among measures of incontinence severity in women undergoing surgery for stress urinary incontinence. J Urol. 2007; 177: 1810-4.
- Hsieh GC, Klutke JJ, Kobak WH: Low valsalva leak-point pressure and success of retropubic urethropexy. Int Urogynecol J Pelvic Floor Dysfunct. 2001; 12: 46-50.
- Hutchings A, Griffiths J, Black NA: Surgery for stress incontinence: factors associated with a successful outcome. Br J Urol. 1998; 82: 634-41.
- Rodríguez LV, de Almeida F, Dorey F, Raz S: Does Valsalva leak point pressure predict outcome after the distal urethral polypropylene sling? Role of urodynamics in the sling era. J Urol. 2004; 172: 210-4.
- O’Connor RC, Nanigian DK, Lyon MB, Ellison LM, Bales GT, Stone AR: Early outcomes of mid-urethral slings for female stress urinary incontinence stratified by valsalva leak point pressure. Neurourol Urodyn. 2006; 25: 685-8.
- Porena M, Costantini E, Frea B, Giannantoni A, Ranzoni S, Mearini L, et al.: Tension-free vaginal tape versus transobturator tape as surgery for stress urinary incontinence: results of a multicentre randomised trial. Eur Urol. 2007; 52: 1481-90.
- Baden WF, Walker T: Grading Support Loss: The Halfway System. In: Baden WF, Walker T (eds.), Surgical Repair of Vaginal Defects. Philadelphia, Lippincott. 1992; pp. 13-23.
- Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, et al.: The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol. 1996; 175: 10-7.
- Pajoncini C, Rosi P, Morcellini R, Costantini E, Mearini E, Guercini F, et al.: Guidelines for endocavity ultrasound scan in SUI and pelvic floor disease. Neurourol Urodyn. 1998; 17: 372-3.
- Ingelman-Sundberg A, Ulmsten U: Surgical treatment of female urinary stress incontinence.Contrib Gynecol Obstet. 1983; 10: 51-69.
- Giannantoni A, Di Stasi SM, Cucchi A, Mearini E, Bini V, Porena M: Pelvic floor muscle behavior during Valsalva leak point pressure measurement in males and females affected by stress urinary incontinence. J Urol. 2003; 170: 485-9.
- Wan J, McGuire EJ, Bloom DA, Ritchey ML: Stress leak point pressure: a diagnostic tool for incontinent children. J Urol. 1993; 150: 700-2.
- Leach GE, Dmochowski RR, Appell RA, Blaivas JG, Hadley HR, Luber KM, et al.: Female Stress Urinary Incontinence Clinical Guidelines Panel summary report on surgical management of female stress urinary incontinence. The American Urological Association. J Urol. 1997; 158: 875-80.
- Cetinel B, Demirkesen O, Onal B, Akkus E, Alan C, Can G: Are there any factors predicting the cure and complication rates of tension-free vaginal tape? Int Urogynecol J Pelvic Floor Dysfunct. 2004; 15: 188-93.
- Abdel-Hady el-S, Constantine G: Outcome of the use of tension-free vaginal tape in women with mixed urinary incontinence, previous failed surgery, or low valsalva pressure. J Obstet Gynaecol Res. 2005; 31: 38-42.
- Jeon MJ, Chung DJ, Park JH, Kim SK, Kim JW, Bai SW: Surgical Therapeutic Index of Tension-Free Vaginal Tape and Transobturator Tape for Stress Urinary Incontinence. Gynecol Obstet Invest. 2007; 65: 41-46.
- Guerette NL, Bena JF, Davila GW: Transobturator slings for stress incontinence: using urodynamic parameters to predict outcomes. Int Urogynecol J Pelvic Floor Dysfunct. 2008; 19: 97-102.
- Lowenstein L, Dooley Y, Kenton K, Rickey L, FitzGerald MP, Mueller E, at al.: The volume at which women leak first on urodynamic testing is not associated with quality of life, measures of urethral integrity or surgical failure. J Urol. 2007; 178: 193-6.
____________________
Accepted after revision:
November 26, 2007
_______________________
Correspondence address:
Dr. Massimo Lazzeri
Section of Urology and Andrology
Via Brunamonti 51
06100 Perugia, Italy
Fax: + 390 75 572-6123
E-mail: lazzeri.m@tiscali.it
EDITORIAL COMMENT
The cure of female stress urinary incontinence should be based on proper patient selection in order to improve the outcome and accurately predict the therapeutic results. Over the years, there have been various proposals for therapy design regarding the existence or absence of overactive bladder concomitantly with stress urinary incontinence, urethral hypermobility or hypomobility, intrinsic sphincter deficiency, etc. The Valsava leak point pressure (VLPP) was previously advocated as an important cure rate predictor for the mid-urethral sling operations, and this may influence the surgeon to elect other operations, such as one of the tension free vaginal tape (TVT) like ones. This might lead the patient to lose the overall TVT benefits and suffer some of the previously used operative modalities. This study evaluates the real value of the VLPP for the prediction of success rate with both TVT and transobturator tape (TOT), with clear and objective tools. Even though being retrospective, the additional information provided here for the urogynecologist practitioner makes the selection of operations for patient free of bias.
Dr.
M. Neuman
Urogynecology, Department of Gynecology
Shaare Zedek Medical Center
Ben-Gurion University of the Negev
Jerusalem, Israel
E-mail: neuman@szmc.org.il
EDITORIAL COMMENT
Preoperative
urodynamic evaluation is common in women undergoing stress incontinence
surgery. Urodynamic observations have been used to confirm the diagnosis
of urodynamic stress incontinence (USI) by observing transurethral urine
loss at the moment of increased abdominal pressure in the absence of a
detrusor contraction. In addition to this general diagnostic finding,
urodynamic criteria are also used to inform surgical decision-making.
The concept of intrinsic sphincter deficiency (ISD) or type III incontinence
was introduced by McGuire to characterize a urethra that no longer has
a functioning sphincter (1). Commonly used measures to evaluate urethral
sphincter integrity are Valsalva leak point pressure (VLPP) and maximal
urethral closure pressure (MUCP); low values have been associated with
poor surgical results. Previous studies have demonstrated a higher failure
rate of the Burch procedure in patients with a MUCP lower than 20 cm H2O
(2, 3). This cut off value of MUCP ≤ 20 cm H2O has been
used arbitrarily as an indicator for ISD. Other reports have evaluated
sphincter function on the basis of the VLPP, the lowest abdominal pressure
to cause urinary leakage as recorded during a slowly performed Valsalva
maneuver. In the original report by McGuire et al. (4), the VLPP was performed
with the patient standing under fluoroscopy. Their results demonstrated
that 75% of patients with type III incontinence had a low VLPP. A low
VLPP less than 60 cm H2O was thought to be associated with
type III incontinence, which is characterized by an open bladder neck
at rest and an immobile urethra with proximal damage (5).
The value of urethral sphincter functioning
as a predictor for the success rate of tension free vaginal tape (TVT)
and transobturator tape (TOT) is controversial (6-8). Most published studies
have a small number of participants and are under-powered (6-8). Dr. Costantini
and her group should be commended for attempting to answer a clinically
relevant question regarding the prognostic value of VLPP for the success
of midurethral slings. The presented study is an ancillary part of a randomized
study which compared TVT vs. TOT for treatment of stress urinary incontinence
(9). All patients underwent standardized multi-channel urodynamic testing
prior to the surgery. VLPP values were obtained at a bladder volume of
200 mL. The patients were randomized to either TVT or TOT irrespective
of the urodynamic results. Overall there were no differences in the cure
rate of patients who had VLPP ≤ 60 cm H2O to those who
had VLPP > 60 cm H2O. A major limitation of this study is
the relatively narrow distribution and low median VLPP of the participants.
The median values for TOT and TVT were 61 and 66 cm H2O respectively.
Since a VLPP around 60 cm H2O is regarded as low, the authors
might have found more significant differences in a group of patients with
a wider distribution of VLPPs. In addition, further evaluation of the
recorded MUCP data as it relates to surgical cure rates could also be
useful. In summary, the ability of urodynamics to predict the success
of SUI surgery is not yet fully recognized and more studies are needed
to elucidate the role of preoperative urodynamics.
REFERENCES
- McGuire EJ, Woodside JR, Borden TA, Weiss RM: Prognostic value of urodynamic testing in myelodysplastic patients. J Urol. 1981; 126: 205-9.
- Bowen LW, Sand PK, Ostergard DR, Franti CE: Unsuccessful Burch retropubic urethropexy: a case-controlled urodynamic study. Am J Obstet Gynecol. 1989; 160: 452-8.
- Quadri G, Magatti F, Belloni C, Barisani D, Natale N: Marshall-Marchetti-Krantz urethropexy and Burch colposuspension for stress urinary incontinence in women with low pressure and hypermobility of the urethra: early results of a prospective randomized clinical trial. Am J Obstet Gynecol. 1999;181: 12-8.
- McGuire EJ, Fitzpatrick CC, Wan J, Bloom D, Sanvordenker J, Ritchey M, Gormley EA: Clinical assessment of urethral sphincter function. J Urol. 1993; 150: 1452-4.
- Blaivas JG, Olsson CA: Stress incontinence: classification and surgical approach. J Urol. 1988; 139: 727-31.
- O’Connor RC, Nanigian DK, Lyon MB, Ellison LM, Bales GT, Stone AR: Early outcomes of mid-urethral slings for female stress urinary incontinence stratified by valsalva leak point pressure. Neurourol Urodyn. 2006; 25: 685-8.
- Bai SW, Jung YH, Jeon MJ, Jung DJ, Kim SK, Kim JW: Treatment outcome of tension-free vaginal tape in stress urinary incontinence: comparison of intrinsic sphincter deficiency and nonintrinsic sphincter deficiency patients. Int Urogynecol J Pelvic Floor Dysfunct. 2007; 18: 1431-4.
- Miller JJ, Botros SM, Akl MN, Aschkenazi SO, Beaumont JL, Goldberg RP, Sand PK: Is transobturator tape as effective as tension-free vaginal tape in patients with borderline maximum urethral closure pressure? Am J Obstet Gynecol. 2006; 195: 1799-804.
- Porena M, Costantini E, Frea B, Giannantoni A, Ranzoni S, Mearini L, Bini V, Kocjancic E: Tension-free vaginal tape versus transobturator tape as surgery for stress urinary incontinence: results of a multicentre randomised trial. Eur Urol 2007;52:1481-1491.
Dr.
Lior Lowenstein
Division of Female Pelvic Medicine
& Reconstructive Surgery
Dep. of Obstetrics & Gynecology and Urology
Loyola University Medical Center
Maywood, Illinois, USA
E-mail: llowenstein@lumc.edu
EDITORIAL COMMENT
The
current study, “Preoperative Valsava Leak Point Pressure May Not
Predict Outcome of Mid-Urethral Slings. Analysis from a Randomized Controlled
Trial of Retropubic versus Transobturator Mid-Urethral Slings” by
Costantini et al is a well designed, randomized controlled trial attempting
to address a valuable clinical issue.
Overall, the use of a trans-obturator approach
(TOT) for mid-urethral sling can minimize the risk of injury to the lower
urinary tract. It has been found to be equally efficacious compared to
the retropubic approach (TVT) in the management of stress urinary incontinence
for patients with normal urethral function. If this were also true for
patients with poor urethral function, or intrinsic sphincteric deficiency
(ISD), universal use of the trans-obturator approach may be preferable.
However, the current study must be evaluated
critically, and its potential flaws recognized. The optimal definition
of ISD is disputed. Many clinicians prefer the use of static maximum urethral
closure pressure (MUCP); studies have shown a wide discrepancy between
MUCP and VLPP. Additionally, the study is underpowered. With only 50 patients
in the ISD group, and an 8% difference in objective cure with TVT showing
superiority, any definitive conclusions cannot be reached.
The authors’ study is a valid first
attempt to address a vital clinical issue in how best to triage and manage
our at-risk patients undergoing anti-incontinence surgery. Though the
universal use of the potentially lower-risk TOT may indeed prove true,
the practice warrants further study before being widely adopted.
Dr.
Kenneth Powers
Associate Professor Obstetrics & Gynecology
Albert Einstein College of Medicine
Chief of Urogyneocology
Montefiore Medical Center
Bronx, New York, USA
E-mail: hoppowers@aol.com