TRANSPERITONEAL
LAPAROSCOPIC PYELOPLASTY: BRAZILIAN INITIAL EXPERIENCE WITH 55 CASES
(
Download pdf )
MARCO T. C. LASMAR, HILARIO A. CASTRO JUNIOR, ALESSANDRO VENGJER, FRANCISCO A. T. GUERRA, EUGENIO A. C. SOUZA, LYDSTON M. ROCHA
Felicio Rocho Hospital, Belo Horizonte, Minas Gerais, Brazil
Clinical Urology
Vol. 36 (6):
678-684, November - December, 2010
doi: 10.1590/S1677-55382010000600005
ABSTRACT
Purpose:
To evaluate prospectively the results obtained in 55 patients undergoing
laparoscopic pyeloplasty through transperitoneal access.
Materials and Methods: From January 2005
to July 2009, fifty-five patients between 13 and 64 years old, were treated
for ureteropelvic junction (UPJ) stenosis via a transperitoneal laparoscopy.
All patients had clinical symptoms of high urinary obstruction and hydronephrosis
confirmed by imaging methods. Anderson-Hynes dismembered pyeloplasty was
performed in 51 patients and Fenger technique in the other 4 cases. Patients
were clinically and imaging evaluated in the postoperative period at 3
and 6 months and then followed-up annually.
Results: The operative time ranged from
95 to 270 min. The mean hospital stay was 2 days. The average blood loss
was 170 mL. The time to return to normal activities ranged from 10 to
28 days. Anomalous vessels were identified in 27 patients, intrinsic stenosis
in 23 patients and 5 patients had high implantation of the ureter. Laparoscopic
pyelolithotomy was successfully performed in 6 patients with associated
renal stones. That series monitoring ranged from 1 to 55 months. One patient
had longer urinary fistula (11 days), 3 patients had portal infection
and 6 patients had prolonged ileus. There was one conversion due to technical
difficulties. From the later postoperative complications, 2 patients had
re-stenosis, one determined by Anderson-Hynes technique and the other
by Fenger technique. The success rate was 95.65%.
Conclusions: Laparoscopic pyeloplasty has
functional results comparable to conventional open technique. It offers
less morbidity, with aesthetic and post-operative convalescence benefits
and lower complication rates.
Key
words: kidney; ureter; laparoscopy; pyeloplasty; treatment outcome
Int Braz J Urol. 2010; 36: 678-84
INTRODUCTION
Ureteropelvic
junction (UPJ) obstruction is one of the most common ureter intrinsic
pathologies generally manifested by back pain, renal colic and urinary
tract infection. It can lead to progressive hydronephrosis and renal dysfunction
(1).
The gold standard treatment of this pathology
is Anderson-Hynes dismembered pyeloplasty, traditionally performed in
a conventional open procedure, with success rates over 90% (2).
Minimally invasive techniques, both endoscopic
and percutaneous, with incision of UPJ are also performed with low morbidity,
but with success rates lower than those of conventional surgery (3,4).
Laparoscopic pyeloplasty, first performed by Schuessler et al. (5), in
1993, maintains the principles of open dismembered pyeloplasty, with excellent
functional results and significant reductions in morbidity (6).
The objective of the present a study was
to evaluate prospectively, from the first visit to the follow-up after
surgery, the results obtained in 55 patients undergoing laparoscopic pyeloplasty
by transperitoneal access.
MATERIALS AND METHODS
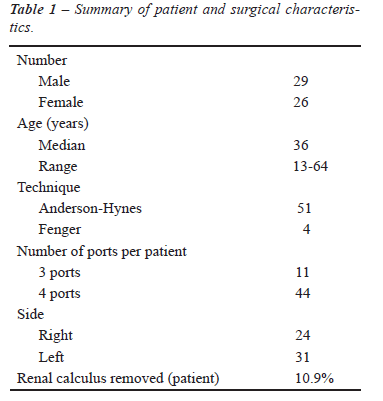
In the period from January 2005 to July 2009, 55 patients, 29 men and 26 women, aged between 13 and 64 years old were treated for UPJ stenosis through transperitoneal laparoscopy by the same surgeon (MTCL). All patients had clinical symptoms of high urinary obstruction and hydronephrosis, confirmed by intravenous urogram and / or multi-slice CT scan. None of them had undergone any previous treatment (Table-1).
Patients were placed in a lateral contralateral
position on the side to be treated. Pneumoperitoneum was made with a Veress
needle and maintained at 15 mmHg. Three or four trocars were placed according
to standard configuration (Figure-1), a paraumbilical one, another between
this one and the ipsilateral iliac crest and the third between that and
the xiphoid appendix. In 44 patients one more trocar was used being located
in the anterior axillary line. A peritoneal incision was made in the line
of Toldt and the colon was medially folded until identifying the ureter
and renal pelvis. Anderson-Hynes dismembered pyeloplasty was performed
in 51 patients and Fenger technique in the other 4 cases. In all cases
was performed a suture of UPJ with 4-0 polyglycolic acid thread in separated
stitches on the spatulated ureter and continuous stitches on renal pelvis.
In 6 cases a lithiasis treatment was made previously identified in imaging
studies, being the calculi successfully removed. The first 15 patients
underwent implantation of double-J stent through retrograde way and in
the others through anterograde way. They were removed after 6 weeks of
surgery. All patients remained with intravesical Foley catheter for 24-48
h and Penrose drain for the same period, except when its drainage persisted.
Patients were clinically assessed and imaging evaluated at 3 and 6 months
and followed annually since then.

RESULTS
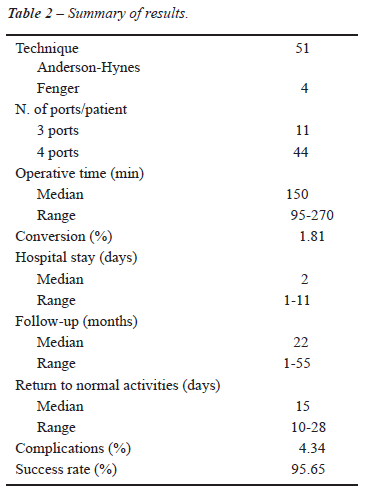
The operative and post-operative results are distributed in Table-2. Mean operative time was 150 minutes (ranging from 95 to 270 min.). There was a progressive decrease in operative time after the first 20 cases. The average blood loss was 170 mL (60 to 370 mL), measured by the content aspirated that may have contained urine. The mean hospital stay was 2 days (1 to 11 days). The average time to return to normal activities was 15 days (10 to 28 days).
Anderson-Hynes dismembered pyeloplasty was
performed in 51 patients and Fenger plasty in 4. Anomalous vessels were
identified in 27 patients (49.09%), ureter intrinsic stenosis in 23 patients
(41.81%) and 5 patients (9.09%) had ureter high implantation. Laparoscopic
pyelolithotomy was successfully performed in 6 patients with associated
calculi, with greater opening of the renal pelvis and using the laparoscopic
equipment.
This series follow-up ranged from 1 to 55
months. Forty-six patients had more than 6 months of follow-up, with complete
resolution of pain observed in 44 of these (95.65%), except for two cases
where re-stenosis was detected in postoperative follow-up period.
There was conversion to open surgery in
a 13-year-old patient due to technical difficulties, in a case carried
out at the beginning of this series. One patient had urinary fistula,
which lasted 11 days, 3 patients had portal infection and 6 patients had
prolonged ileus. All these minor complications were treated conservatively
with complete resolution. From the later postoperative complications,
2 patients (4.35%), over six months of follow-up, showed re-stenosis,
one in which the surgery was performed through Anderson-Hynes technique
and the other through Fenger technique. These complications were identified
at 8 and 4 months of follow-up respectively by low back pain after drinking
water and was confirmed by imaging methods. The first was treated by retrograde
endopyelotomy and the second by open pyeloplasty, both with success.
COMMENTS
Since
its description in 1949 by Anderson-Hynes, open dismembered pyeloplasty
has been the gold standard for UPJ obstruction treatment, with success
rates exceeding 90% (2). The lumbar incision adopted most of the time
(lumbotomy), among other factors, leads to higher morbidity in the procedure,
mainly related to the use of analgesics postoperatively and worse cosmetic
effect besides a longer period of convalescence (6).
Minimally invasive procedures have emerged
with the aim of reducing the morbidity in the open surgery. Retrograde
and anterograde endopyelotomy, pneumatic balloon dilatation, Acucise,
cold Knife and more recently the use of laser were used for the purpose
of treatment of UPJ stenosis. Such procedures have low morbidity, but
lower rates of success (3,4). Moreover, there is evidence that patients
with large renal pelvis, poor kidney function and anomalous vessel are
not good candidates for endoluminal techniques. Added to this, the long-term
results are also worse, at around 63% with more frequent relapses (7).
Initially accepted with difficulty due to
the long operative period and the need for advanced laparoscopic skills,
video-assisted pyeloplasty decreased morbidity and improved cosmetic effect
while maintaining success rates similar to those of the conventional open
technique (1).
Anderson-Hynes dismembered technique is used in most series of published
laparoscopic pyeloplasties, reflecting an attempt to reproduce the well-established
principles of open surgery (6,8), besides being more effective than other
minimally invasive procedures (3,4,7). The dismembered technique should
always be considered, even in the presence of anomalous vessel, because
in more than half of the cases there is an associated intrinsic stenosis
(9).
Laparoscopic pyeloplasty can be performed
by either trans or retroperitoneal approach. Although, the transperitoneal
approach provides more working space for dissection and suturing with
more defined anatomical references, retroperitoneoscopy promotes direct
access to UPJ with less need for dissection and without violating the
peritoneal envelope (10). Both operative time and the results of transperitoneal
way are comparable to retroperitoneal access (11).
When evaluating the results based on the
used ways, both the transperitoneal and retroperitoneal approaches offer
similar success rates, with similar rates of complications (12-18), varying
the choice according to surgeon’s preference and experience.
There was a significant and progressive
decrease in the operative time during this series, associated with greater
experience acquired by the surgeon (MTCL), observing a final average time
of 150 min. In the literature several series of video-laparoscopic pyeloplasty
are described where there is evidence that the time varied from 77 to
312 min with progressive reduction in the postoperative period as it increases
the number of cases, due to the learning curve (18). There was also a
decrease in blood loss with the progression of the learning curve and
therefore it was not necessary to perform blood transfusion in any patient.
Conversion was necessary in one patient
in this series due to technical difficulties. The patient was 13 years
old and was operated in the beginning of the presented series. The conversion
rate was 1.81%, consistent with other series described in the literature.
(17,18).
In this study there were two cases of re-stenosis (4.34%), one performed
through Fenger technique and the other through Anderson-Hynes. Reports
of re-stenosis in the literature ranged from 3.5 to 4.8% of the cases
with the use of Anderson-Hynes technique (18). We must consider that in
open surgery the rates are similar and Fenger technique, itself, has higher
rates of re-stenosis (2). Re-stenosis can be treated by laparoscopic approach,
with success rates similar to those of primary obstruction (19). In our
cases, re-stenosis was operated by open surgery because they occurred
at the beginning of the surgeon’s learning curve. Intraoperative
complications are rare during laparoscopic pyeloplasty as well as postoperative
complications, with rates ranging from 2% to 15% (18,20,21). Complications
in this series were limited, totaling 10.9%, which were a urinary fistula
that lasted 11 days in one patient, three other patients who had operative
wound infection and two cases of re-stenosis.
Open pyeloplasty has been the gold standard
for the treatment of UPJ stenosis since its establishment, with long-term
success rates higher than 90% (2). However, its morbidity is high especially
related to chronic pain, risk of incisional hernia and later return to
‘daily activities’ (6). The success rates of laparoscopic
pyeloplasty were comparable to those of open surgery with long-term rates
as high as 98% (12-18).
In this series, there was a success rate
of 95.65%, consistent with the data presented in the literature for laparoscopic
and open pyeloplasty Table-3.

Since its first report by Sung et al. (22),
pyeloplasty has been performed also assisted by robotics, with results
similar to laparoscopic procedures and standard open surgery. The most
recent reports show a lower learning curve and shorter operative time,
resulting mainly from a higher skill in surgery and simplification of
suture (23), besides the opportunity to perform the treatment of bilateral
pathology cases at once, with practicality, safety and without functional
loss (24). The costs of robotic surgery are major limitations to the procedure
application in several centers.
CONCLUSIONS
Laparoscopic pyeloplasty has functional results comparable to the conventional open technique and better than the other endoluminal procedures. It is a safe and effective alternative for the treatment of pyeloureteral junction stenosis and it can be considered as first choice by surgeons with experience in laparoscopy. The complication rates are low and concurrent procedures, as pyelolithotomies, can be performed.
CONFLICT OF INTEREST
None declared.
REFERENCES
- Inagaki T, Rha KH, Ong AM, Kavoussi LR, Jarrett TW: Laparoscopic pyeloplasty: current status. BJU Int. 2005; 95(Suppl 2): 102-5.
- Persky L, Krause JR, Boltuch RL: Initial complications and late results in dismembered pyeloplasty. J Urol. 1977; 118: 162-5.
- Motola JA, Badlani GH, Smith AD: Results of 212 consecutive endopyelotomies: an 8-year followup. J Urol. 1993; 149: 453-6.
- Nadler RB, Rao GS, Pearle MS, Nakada SY, Clayman RV: Acucise endopyelotomy: assessment of long-term durability. J Urol. 1996; 156: 1094-7; discussion 1097-8.
- Schuessler WW, Grune MT, Tecuanhuey LV, Preminger GM: Laparoscopic dismembered pyeloplasty. J Urol. 1993; 150: 1795-9.
- Bauer JJ, Bishoff JT, Moore RG, Chen RN, Iverson AJ, Kavoussi LR: Laparoscopic versus open pyeloplasty: assessment of objective and subjective outcome. J Urol. 1999; 162: 692-5.
- Brooks JD, Kavoussi LR, Preminger GM, Schuessler WW, Moore RG: Comparison of open and endourologic approaches to the obstructed ureteropelvic junction. Urology. 1995; 46: 791-5.
- Rodrigues H, Rodrigues P, Ruela M, Bernabé A, Buogo G: Dismembered laparoscopic pyeloplasty with antegrade placement of ureteral stent: simplification of the technique. Int Braz J Urol. 2002; 28: 439-44; discussion 445.
- Mitre AI, Brito AH, Srougi M: Laparoscopic dismembered pyeloplasty in 47 cases. Clinics (Sao Paulo). 2008; 63: 631-6.
- Janetschek G, Peschel R, Frauscher F: Laparoscopic pyeloplasty. Urol Clin North Am. 2000; 27: 695-704. Erratum in: Urol Clin North Am. 2001; 28: xi. Franscher F [corrected to Frauscher F].
- Rassweiler JJ, Seemann O, Frede T, Henkel TO, Alken P: Retroperitoneoscopy: experience with 200 cases. J Urol. 1998; 160: 1265-9.
- Jarret TW, Fabrizio MD, Lamont DJ: Laparoscopic peloplasty: five-year experience. J Urol. 1999; 161: 24(suppl.), abstract #79.
- Soulié M, Salomon L, Patard JJ, Mouly P, Manunta A, Antiphon P, et al.: Plante P: Extraperitoneal laparoscopic pyeloplasty: a multicenter study of 55 procedures. J Urol. 2001; 166: 48-50.
- Türk IA, Davis JW, Winkelmann B, Deger S, Richter F, Fabrizio MD, et al.: Laparoscopic dismembered pyeloplasty--the method of choice in the presence of an enlarged renal pelvis and crossing vessels. Eur Urol. 2002; 42: 268-75.
- Sundaram CP, Grubb RL 3rd, Rehman J, Yan Y, Chen C, Landman J, et al.: Laparoscopic pyeloplasty for secondary ureteropelvic junction obstruction. J Urol. 2003; 169: 2037-40.
- Mandhani A, Kumar D, Kumar A, Kapoor R, Dubey D, Srivastava A, et al.: Safety profile and complications of transperitoneal laparoscopic pyeloplasty: a critical analysis. J Endourol. 2005; 19: 797-802.
- Moon DA, El-Shazly MA, Chang CM, Gianduzzo TR, Eden CG: Laparoscopic pyeloplasty: evolution of a new gold standard. Urology. 2006; 67: 932-6.
- Rassweiler JJ, Teber D, Frede T: Complications of laparoscopic pyeloplasty. World J Urol. 2008; 26: 539-47.
- Brito AH, Mitre AI, Srougi M: Laparoscopic pyeloplasty in secondary obstruction. J Endourol. 2007; 21: 1481-4.
- Shoma AM, El Nahas AR, Bazeed MA: Laparoscopic pyeloplasty: a prospective randomized comparison between the transperitoneal approach and retroperitoneoscopy. J Urol. 2007; 178: 2020-4; discussion 2024.
- Vijayanand D, Hasan T, Rix D, Soomro N: Laparoscopic transperitoneal dismembered pyeloplasty for ureteropelvic junction obstruction. J Endourol. 2006; 20: 1050-3.
- Sung GT, Gill IS, Hsu TH: Robotic-assisted laparoscopic pyeloplasty: a pilot study. Urology. 1999; 53: 1099-103.
- Gettman MT, Peschel R, Neururer R, Bartsch G: A comparison of laparoscopic pyeloplasty performed with the daVinci robotic system versus standard laparoscopic techniques: initial clinical results. Eur Urol. 2002; 42: 453-7; discussion 457-8.
- Freilich DA, Nguyen HT, Borer J, Nelson C, Passerotti CC: Concurrent management of bilateral ureteropelvic junction obstruction in children using robotic-assisted laparoscopic surgery. Int Braz J Urol. 2008; 34: 198-204; discussion 204-5.
____________________
Accepted after revision:
March 15, 2010
_______________________
Correspondence address:
Dr. Marco Túlio Coelho Lasmar
Felício Rocho Hospital
Rua Timbiras, 3642, Salas 701/703
Belo Horizonte, MG, 30140-062, Brazil
E-mail: lasmar.uro@uol.com.br
EDITORIAL COMMENT
This
article reinforces that excellent results of laparoscopic pyeloplasty
can be consistently obtained by many authors. In those services with experience
in laparoscopy, it is considered the standard of care for relieving all
conditions related to pyeloureteral junction obstruction for adults and
older children.
The rate of success of Anderson-Hynes dismembered pyeloplasty has duplicated
that of open surgery with incomparable less invasiveness. The endopyelotomy
(transureteral, percutaneous or by Acucise catheter) showed reduced results
when compared to conventional or laparoscopic pyeloplasty and for this
reason is nowadays much less used.
Transperitoneal or retroperitoneal access is no longer a concern but much
more a preference for surgeons. Laparoscopic pyeloplasty has shown to
be an excellent option for secondary pyeloureteral obstruction as considered
in discussion. Removal of renal associated stones may depend on intra-renal
location, size, number of stones, and the anatomy of the urinary tract
and the rate of success is not uniform. Flexible nephroscope may be an
important tool to retrieve calyceal stone not approachable using rigid
lens, leaving more kidneys stone free.
When available, in my opinion, the assistance of the Da Vinci robot may
become laparoscopic pyeloplasty accessible for all urologists particularly
those with no experience with laparoscopic procedure.
Dr.
Anuar I. Mitre
University of Sao Paulo, USP
Sao Paulo, Brazil
E-mail: anuar@mitre.com.br